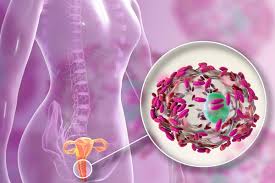
Under normal conditions, many microorganisms are physiologically present in the vagina, the most common of which are Lactobacillus crispatus and Lactobacillus jensenii. Lactobacilli help prevent the excessive growth of other microorganisms by maintaining a balanced vaginal flora. Microorganisms capable of causing vaginosis are diverse, and among them Gardnerella vaginalis should be mentioned first.
An imbalance of the bacterial flora associated with a decrease in the number of lactobacilli, which may be caused, for example, by the use of antibiotics or disruption of the pH balance, allows more resistant bacteria to colonize and multiply.
Bacterial vaginosis caused by Gardnerella may be associated with sexual activity, but there is no clear evidence of sexual transmission. However, the incidence is higher among sexually active women aged 15 to 50, and in some cases postmenopausal women are also affected by Gardnerella.
How does it manifest?
Approximately half of the women suffering from this condition have no symptoms, but if they do appear, the characteristic signs of Gardnerella infection are a specific vaginal odor and white-gray discharge. The unpleasant smell is often described as “fishy,” much more intense than usual, and it is noticeable immediately, especially after sexual intercourse. Its intensity may vary, but it is still easily recognizable. The infection usually does not cause pain or itching.
Gardnerella in men
Gardnerella is usually transmitted to men from their sexual partners. In men, gardnerellosis usually occurs without symptoms, and the patient most often does not know about the infection. A condom is usually a sufficient precaution to prevent infection, along with certain hygiene measures, such as avoiding the use of shared towels for intimate hygiene. Treatment usually includes the same substances used for women, possibly also with topical creams.
What are the risks?
Sexually transmitted infections (STIs) that may develop after inadequate treatment of vaginosis are often more serious and more difficult to treat. Some risks are associated with this condition, including: a higher likelihood of infection after procedures such as hysterectomy or abortion; increased susceptibility to other sexually transmitted diseases such as herpes simplex, chlamydia, and gonorrhea. Pregnant women with Gardnerella or other forms of vaginosis more often experience premature birth and give birth to babies with low birth weight. Gardnerella can, in some cases, infect the uterus and fallopian tubes. This condition increases the risk of ectopic pregnancy and infertility in the future.
What should be done?
The main goal of treatment is not only to eliminate Gardnerella but also to restore the physiological acid-base balance of the vagina. Although in some cases the disease may resolve spontaneously, treatment is strongly recommended to relieve symptoms and prevent complications, especially before surgical procedures or during pregnancy. Specialists from the Bogolyuby Medical Center emphasize that antibiotics remain the cornerstone of treatment. The use of vaginal acidifying agents, namely gels with lactic acid, can help restore the pH to a normal level, creating an environment unfavorable for Gardnerella.
Unfortunately, Gardnerella vaginosis recurs in more than 30% of women within several months. Therefore, after antibiotic therapy it is recommended to take certain strains of lactobacilli, for example L. rhamnosus or L. reuteri, to restore the vaginal microflora and reduce the risk of recurrence.
From a lifestyle perspective, it is important to stop douching, which “destroys” beneficial bacteria, and to use intimate hygiene products with an acidic pH (3.5–4.5). During treatment, it is recommended to abstain from sexual intercourse or consistently use condoms until the symptoms completely disappear.
Number of views: 172